Less than 4 weeks ago, I wrote a blog post about Blue Cross and Blue Shield of Georgia’s new policy to deny Emergency Room visits later determined not to have been an emergency. At the end of last month, it was reported that Anthem, the parent company of Blue Cross and Blue Shield, has implemented yet another policy aimed at curbing expenses. They will no longer pay for outpatient CT and MRI scans done in hospitals without prior approval. For now, the policy impacts subscribers in Indiana, Wisconsin, Missouri, Kentucky, and Ohio, but many speculate it will spread to other states. There is certainly a need to curb healthcare costs in the United States. However, will patients get caught in the middle of the fight between insurers and hospitals? In this article, I give you some tips to navigate this minefield and avoid being left with a huge bill.
*I recorded a Facebook Live video on this topic on 10/8/18. To check it out, click here.
Let’s start with the medical terminology.
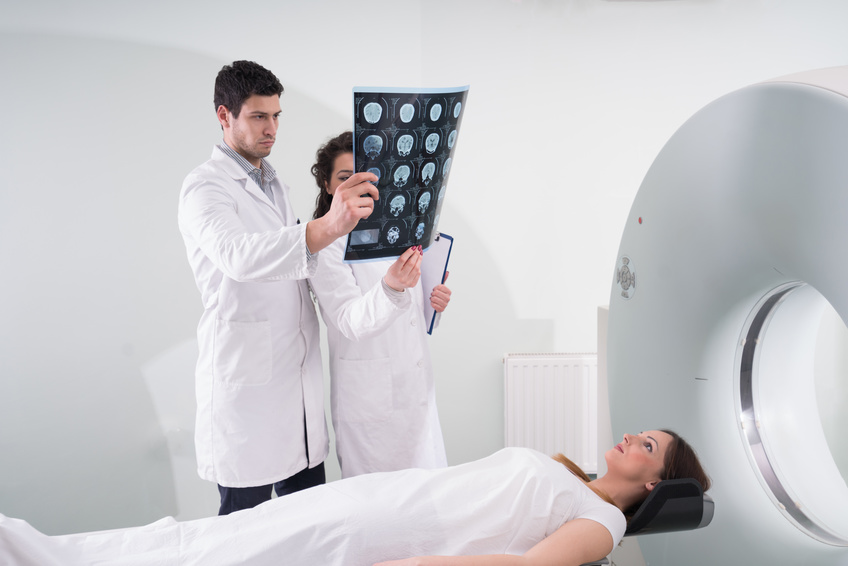
A CT scan, otherwise known as a “CAT scan”, is essentially a very fancy X-ray. X-ray measurements are taken at various angles, then processed by a computer to produce cross-sectional images of body parts. These images allow physicians to detect internal injuries, infection, cancer, and other abnormalities in great detail. An MRI scan uses magnetic energy to take cross-sectional images of organs and structures inside the body. It provides even greater detail than a CT scan, does not require the use of radiation, and is often the preferred study for imaging the brain and spinal cord.
Enough of the medical mumbo-jumbo. Let’s get to the heart of the issue—money.
These scans cost a lot of money. According to various sources, the cost of a CT scan in the U.S. can range from $270-$2800 and the cost of an MRI scan can range from $400 to $3500. To understand the reason for these broad price ranges, you need to know what’s included in the bill. There are 3 fees included in the bill for imaging studies: 1) the technical fee, 2) the professional fee, and 3) the facility fee. The technical fee is the fee for the procedure itself. This price varies, depending on the body part being imaged. For example, imaging studies of the brain are more expensive than studies of the abdomen. The professional fee is for the physician (radiologist) who interprets the study. Lastly, there is the facility fee, which is at the root of Anthem’s decision. It turns out there is huge variability in what is charged, based on whether the test is done in a hospital or a freestanding outpatient facility.
According to www.amino.com, the average cost of an MRI is $787 at a freestanding radiology facility and $1767 at a hospital; a difference of almost $1000! One of the reasons hospitals charge more is to offset the costs of operating a business that is open 24 hours/day, 7 days/week. Another reason hospitals charge more is to offset the losses from other services provided, such as those that are less profitable or free/charity care. Finally, hospitals charge more because they can. Now that you see how much more it costs to get outpatient MRI and CT scans in a hospital, you can begin to understand why insurance companies like Anthem are placing restrictions and are mandating that non-emergent studies are done outside of the hospital setting. In many cases, this is an appropriate decision. However, it just wouldn’t be the U.S. healthcare system if things were that simple.
Patients with chronic diseases are worried about this new policy. Imagine you are a cancer survivor who gets CT scans every 3-6 months to ensure the cancer is still in remission. All of your specialists are at the local academic medical center. For the last 18 months, you have had your CT scans done at that hospital. You and your doctors have been happy with this process, as they have access to your results within hours of the study being completed and the transfer of information is seamless. Under the new policy, there is a good chance you will be forced to have your CT scan at a free-standing facility. What’s wrong with that, you may ask? One concern is that the radiologist at the freestanding facility may not have extensive experience with your form of cancer. This can potentially impact the accuracy of the study results. In addition, while your doctor will get a report from the radiologist, he will not be able to personally review the scans because the electronic medical records of the two facilities are not compatible with one another. You will now have to request a copy of your scan (which typically takes several days), then take it with you to the academic medical center so your specialists can review the actual images.
Patients who live in remote rural areas are also concerned about the new policy. For some, the closest freestanding radiology facility is over 100 miles away. For individuals who own a car and are in relatively good health, the worst consequence may be that this will cause a significant inconvenience. For individuals with disabilities or those who rely on public transportation, the barriers may be deemed insurmountable and the patient just won’t get the test.
What does pre-authorization entail?
According to Anthem’s FAQ page, CT and MRI requests will be subject to a “medical necessity review”. The purpose of this review is to determine whether a particular diagnostic test or treatment is appropriate and essential. Decisions are made based on the standard of care and the individual health plan’s policies and clinical guidelines. If Anthem determines that it is medically necessary for the scan to be done in a hospital, the procedure will be approved. If not, the request will be denied and the ordering physician will need to send the patient to a freestanding outpatient facility. You have the right to appeal insurance denials, particularly if your physician disagrees with the decision. (Please read How to File an Appeal When Your Insurance Company Refuses to Pay for more information.)
What should you do as a healthcare consumer?
It is critically important to review the terms of your health insurance contract in order to understand how these types of policies will affect your bank account. No one wants to receive a surprise bill for a service they thought was covered. In some circumstances, if a CT or MRI is completed in a hospital without proper pre-authorization, the insurance company will not pay the claim but the patient is not responsible for the charges. However, in other cases, you may be liable for the entire bill. Even if your insurance company does not yet have a policy that requires pre-authorization for MRI and CT scans, if you have a PPO (provider-preferred organization) or high-deductible health plan in which you are responsible for a portion of the costs, your out-of-pocket expenses will be dramatically higher when these studies are performed in a hospital. (For a review of the types of insurance plans, please read How to Choose the Health Insurance Plan That’s Best for You.)
There is no doubt that the Anthem policy and others like it will be adopted by other insurance companies across the United States. If you don’t want to be a victim in this cost-cutting war, you will need to arm yourself with information that will empower you to be proactive and to advocate for yourself.
There are three questions you should ask if your doctor orders a CT or MRI scan: 1) Ask why the test is being ordered so you have a clear understanding of what the doctor is looking for. 2) Ask whether you are being sent to a hospital or a free-standing facility. If the test is to be completed at a hospital, ask your doctor if she thinks it is appropriate for you to have the study at a freestanding facility. If your doctor recommends that you have the scan at a hospital, trust her judgment. 3) BEFORE you schedule the appointment for the scan, contact your health insurance provider (or you can review your policy documents online or in print) to determine if pre-authorization is required. If required, make sure this has been completed prior to getting the scan. Following these steps will help you partner with your doctor and minimize your chances of being caught off guard with an astronomical bill.
*We had a riveting discussion about this topic on Navigator Nuggets, my weekly Facebook Live show. To see the video click here.
Have you joined the Your GPS Doc Family? If not, please click here to receive notifications about new content as well as useful guides and additional resources only available to Your GPS Doc subscribers.






It’s really great to know this information. It’s really authentic and usable thoughts. Thank you for sharing.
I am going through this right now. My CT scan was scheduled for tomorrow at a hospital and my insurance company did not authorize so the hospital cancelled my appointment. Doctor’s office talked with the insurance company and provided them with whatever they asked for. I have to wait till Monday to find out whether or not they will authorize. And if not I will have to get x-ray or ultrasound done.
I am so sorry. Hopefully, they will approve the request now that they have additional information from your doctor. Ultimately, they may approve the test but they may require that you have it done at an outpatient facility instead of a hospital. The cost difference can be huge!
And if they see something in those tests, the insurance company will have the evidence that a CT scan is needed. So I have waited over a month now already and maybe I will have to wait another month or longer just to find out whether or not I have cancer. That is so messed up. Why are they asking for evidence for the need of this test? The test is to find out what is wrong. How can anyone know what is wrong without the test result? I have low wbc (it was Normal in January) and I have 7-8 swollen lymph nodes in my neck for over 5 weeks now. Isn’t that enough reason for a concern? I am so stressed already and the insurance company is making is worse.
Oh my goodness, I’m sure this is very stressful for you. Please be diligent about following up with the request. Unfortunately, there is often a disconnect between patient care and the insurance companies who pay for it. I wish you the best of luck.
Thank you! There is a 90% chance that I do not have cancer. I am trying to think positive. It’s just that I was so close to finding out and the process delayed last minute. My doctor and his staff are very helpful so I am sure it will work out eventually. Hoping for the best.
My father has been sick for years. Years of random vomiting, sweats, the whole 9 yards. Insurance will still not approve CT scan. Wtf
Wow, Toni. I’m so sorry.
I’m running into issues with this as we speak. Anthem BCBS apparently uses a secondary company to determine whether a CT scan is needed. I have a softball-sized mass in my abdomen that was identified in an x-ray, after I complained about consistent abdominal discomfort that’s been going on for months. This company determined that a CT scan was NOT NECESSARY. My doctor now needs to contact the company to have a peer-to-peer review with their doctor about why it’s necessary for me to have this scan. If I hadn’t just spent the last week not sleeping while worrying about this, I’d laugh.
I would never, EVER use this insurance company by choice.
Heather, I am so sorry to hear this. It is very frustrating when insurance companies get in the way of appropriate medical care. I’m sure your doctor will advocate for you during the peer-to-peer review. I wish you the best of luck and I hope you get a speedy resolution to your problem. Thank you very much for reading and sharing your thoughts.
What happens if the last appeal is denied? My boyfriend has a similar issue. He needs the scan or they won’t perform surgery. Is it possivle to get the scan and pay out of pocket? Will the doctor use the scan?
Hi Amanda,
I’m sorry to hear about your boyfriend. You can always pay out of pocket for a CT scan. You can then request a copy of the scan to bring to your physician. I recommend that your boyfriend call around to compare prices, as they can vary greatly between radiology facilities. Scans performed in outpatient free-standing facilities will generally be cheaper than those performed in a hospital. However, if the scan is needed for surgery he needs to talk with the surgeon about acceptable places to get the scan, as the surgeon may have requirements that cannot be met by all facilities.
Denied ? $1700 a month that’s hardly used . One of these days everyone is going on strike ! They make a fortune! All about $$&& I bet no one in there family gets denied . They should trust the Dr. they need to be sued by anyone that dies because of being denied. Life is hard enough bring in pain and being denied of a test because of $ is a crime ! KARMA
Yes my wife died waiting for pet scan after haveing CT scan. Because insurance denied..they saw spots on lungs ended up in er said pneumonia turned to sepsis then septic shock she died 11/24/17 she had been seeing a lung specialist but was waiting on insurance to allow pet scan
Yes my wife died waiting for pet scan after haveing CT scan. Because insurance denied..they saw spots on lungs ended up in er said pneumonia turned to sepsis then septic shock she died 11/24/17 she had been seeing a lung specialist but was waiting on insurance to allow pet scan
Oh my goodness, how horrible. I am so very sorry for your loss.
So my son had an MRI 3/21/18. We just received notice on 3/30 that it was not approved by insurance pending further information. The MD office sent the PA the same day the MRI was completed-although this test had been scheduled for over 2 months. If insurance denies the MRI (which also included sedation with anesthesia) will we be responsible for the mri, sedation, and anesthesia?
Hi Sarah,
Each insurance company has their own policies regarding prior authorization, but the key word is “prior”. Ideally, you want the request submitted in enough time to allow for an appeal if the procedure is denied. I’m crossing my fingers on your behalf. If it is denied, be sure to solicit the help of your physician to write a strong appeal letter.
my son just turned 17 and has no insurance. the state chip program recently dropped him.
he needs an MRI, can we pay out of pocket?
Hi Joyce,
I am sorry to hear that. You can always pay out of pocket but MRI scans tend to be very expensive. I recommend you talk to his doctor to review your options. If you must pay out of pocket, be sure to call around to various outpatient radiology facilities because price can vary greatly. Check out my article, “Shopping for Healthcare Deals” for more information and good luck!
My insurance company has denied my MRI. Twice now and my story is quite different! I’ve had 3 drs tell me I need a mri and insurance is being very difficult to say the least!! My neuro surgeon mailed me the denial letter and asked me who I pissed off and said they have never heared such ludicrous reasons for the denial! I have had the X-ray and CT already and went thru a painful physical therapy insurance made me go to.( Which I know they always have you jump thru hoops first ). I am no longer able to work at all and the pain and symptoms are getting worse! The insurance company stated it wanted me to quit smoking before they would approve an MRI! Yes you read that right! I know my surgeon wants me to quit but insurance saying I have to and take a urine test proving it ? Also they questioned my results from CT and wanted my dr to explain the results? Which he did ! I called my insurance company and they totally passed the buck and said it was my drs office who hadn’t submitted everything they requested. So they resubmitted it and I was denied again?? I have fragmented discs now and have Been diagnosed with all the major back problems ,stenosis. spondylthesis. Etc
I don’t know what to do? I’m at a stand still and seems like I can’t get any help! And let’s not mention the fact that while I’m waiting I’m living in pain every day and cannot work and because of all the pill popping addicts I cannot get any help managing my pain either!
Teresa, I am so sorry that your insurance company is being uncooperative. As a physician, it really angers me when individuals with no medical training override a physician’s recommendation. Please talk with your physician about filing an appeal. I hope and pray you get relief very soon.
I’ve been in contact with my neuro s office and in fact asked her to resubmit it after I called the insurance company myself after being frustrated from the first letter She said she would do it and then days later called me back and said she had bad news again. I asked her what I can do and where do I go from here and she basically told me good luck and she had exhausted all of her options!? She said I can try my husbands work and have them call the insurance company ? It’s not like they are a huge corporation or anything so I don’t think that would threaten them in anyway. I’ve been reading about insurance commission? And a external review?? I just don’t know how to go about doing that and also I’m so confused by the insurance Mumbo jumbo. Where exactly I’m at in the process? They say one thing then turn around and talk about another ? ? I thought the drs office does a pre treatment notification first ? Well the second letter says a final coverage determination cannot be made until and actual claim is submitted?? I don’t understand that part and my drs office and our conversation yesterday sounded like she was done with me? I wish I could post the letters. You really won’t believe ur eyes!
My drs office says they did file an appeal already?
Nicole is there anyway I can send you the letters? I I would really like ur opinion
Teresa,
I am very sorry for all of the difficulties you are having. As you and I are not in an advocate-client relationship, I am unable to provide you with specific advice. Please consider hiring a private health advocate in your city and I really hope you get this resolved.
Thank you*
I am waiting for prior authorization for an MRI scan for my back. My insurance provider is dragging their feet so I called up the billing department at the hospital that I would have the MRI scan. I told them I was still waiting for my insurance company to approve it, but figured since I had not yet reached my deductible I was more than most likely going to be paying for the exam myself and decided I could just skip the middleman (insurance company) if the scan was within my price range. They quoted me $830 for the MRI and I said great, I can dip into savings and just pay for it out of pocket only to be informed that if I did this without having received prior approval that any procedure related to anything found in the scan would not be covered by my insurance. How is this even legal?!?!?!
Hi Judith,
I am sorry that you are having challenges getting your MRI scan. It seems unusual (and unreasonable) that your insurance company would not cover procedures related to findings of the scan if you pay for it yourself, BUT there is a lot of small print in insurance company contracts that most don’t read. Therefore, I recommend that you speak directly with your insurance provider to clarify this matter. If they are taking a long time to approve the scan, you can ask the physician who ordered it to contact them on your behalf, particularly if your symptoms are worsening. I wish you the best of luck!
My primary had a peer-to-peer and they turned me down for the MRI. Will be going in for an X Ray and finger cross that something shows up that would compel my insurance company to let me have the MRI. What is laughable is they wanted to know what procedure I was getting, surgery, injections, etc… in order to justify the MRI. My doctor explained he could not authorize surgery, injections, etc without knowing what was going on in my back, which was why he needed the MRI in the first place. The whole system is madness!
Best of luck!
I am dealing with a similar issue as everyone else. My primary doctor ordered a MRI of my spine to determine whether my degenerative disc disease has progressed further. My last MRI which led to diagnosis of DDD was maybe three years ago, and at the time my neurologist said it hadn’t progressed to a point where surgery was a good option. Despite this, Cigna denied the MRI even after two peer-to-peer conversations with my doctor.
I am now having debilitating pain and numbness throughout my entire body on a near daily basis that is getting progressively worse. My primary doctor has run blood tests to determine whether I have an autoimmune disease (rheumatoid arthritis, lupus, Lyme). These came back negative. I’ve had a nerve conduction study done to determine why along with the pain I had also lost feeing in my hands and fingers (questionable diagnosis by specialist of carpal tunnel), especially when I also experience this in my legs and feet. I’m also scheduled to see a rheumatologist in two months.
The ridiculous part of this is that Cigna says that I haven’t seen the doctor enough in the past year and a half for this. (??) Even worse is that they now are REQUIRING me to see a physical therapist for an unspecified amount of time before they will reconsider. I CAN BARELY MOVE WITHOUT PAIN, AND THEY WANT ME TO SUBJECT MYSELF TO “THERAPY” THAT WILL NO DOUBT CAUSE EVEN MORE PAIN! For a documented CHRONIC CONDITION. What boggles my mind is that they will cover this, but not the MRI.
Honestly, I just want to find out if my spine is causing the problem before my doctor moves on to further, more invasive and expensive tests for autoimmune issues. I just want feel better and be proactive with my health, and yet it seems Cigna doesn’t want to cooperate. I’m so frustrated.
Hi Kimberly,
I am very sorry you are having severe pain. It is not uncommon for insurance companies to require “conservative management” of certain conditions prior to approving additional studies, such as MRI scans. While you are worried about physical therapy causing more pain, many individuals with chronic pain find that their pain improves with physical therapy. I recommend that you discuss this with your physician to ensure he/she doesn’t have any objections. If your symptoms are not improved with therapy, hopefully your insurance company will promptly approve the MRI. I wish you the best.
I had a STAT CT done at an immediate care. The CT showed a lesion in the posterior fossa. I am now at day 5 waiting for my authorization for the MRI that the neuroradiologist recommended to have done right away. It is currently in peer to peer review. The doctor that ordered the MRI is my PCP. My PCP said he won’t do the peer to peer because he is not a neurologist and won’t be able to answer all their questions. What are the chances that Anthem BC will deny the claim?
Hi Susan,
First of all, I am very sorry you are going through this and will pray for a good outcome re: the MRI results. I can’t tell you the chances Anthem will deny the request but, given the information you’ve provided, an MRI seems like the logical next step. You’d be surprised who’s involved in “peer-to-peer” calls. Often, the physician representing the insurance company is not a specialist in the area of question. I bet your PCP would do a fine job defending the need for the study. I wish you the best of luck.
My mother was diagnosed by a Neurologist with severe Alzheimer’s disease. He ordered an MRI and EEG through the SAME hospital he works in. The Neurologist accepted my mom’s Medicaid Insurance. The Radiology Department however did not. We tried twice in person and twice they denied to see her on her scheduled day for the tests. We called the number for Medicaid and was provided with a list of In Network hospitals that accept Medicaid. We scheduled her MRI and EEG through one of the hospitals recommended by Medicaid. The hospital confirmed that they accepted the insurance. Close to the date of her appt, we got a call. The appt was cancelled because the Neurologist needed to be in Network and working through that hospital. We called the Neurologist and they indicated that the Primary Doctor has to Authorize the MRI and EEG through that hospital. We feel time is of the ESSENCE and we are back to square one. The problem is that my mom has lost her referral from the doctor for the Neurologist. She has a new Doctor and we do not know who she saw. Do we start from scratch and find a new Primary Provider? Do we have rights to have these tests Authorized due to her condition? Any guidance would be extremely helpful.
Hello Claribell,
Wow, it sounds like you all have been through a lot trying to get the MRI and EEG. Pre-authorization is generally required by the insurance company, not the hospital. The hospital must have received notification from Medicaid that the studies would not be covered without pre-authorization, hence the call to cancel the tests. I am not sure why the neurologist needs to be in the hospital’s network. I would contact your mother’s new primary care provider and let him know you need pre-authorization for these studies. I would make sure this new doctor has access to the neurologist’s evaluation of your mother. That should give him all of the information he needs to obtain pre-authorization from the insurance company. Stay in touch with the insurance company to ensure things are moving forward. Be a pest. I wish you the best of luck.
Going through this right now. Blown knee. been waiting a month.
I’m so sorry. I hope you get a resolution soon.
I had a quad bypass 6 months ago. I was told I needed to do 30 mins cardio daily. I was moving a bed upstairs and in the process hurt myself. I suspected a hernia. I went to my doctor who ordered imaging. The insurance turned it down. I contacted the health advocate, what a waste of my time, they told me to appeal. I appealed and was turned down again. This appeal process took weeks, during which time I could not do my cardio and my pain increased. I was in so much pain I was missing work. My left testicle was hurting and I called the company doctor. They suggested I call a surgeon and refused to see me. I called the Tell-a-Doc service. He advised me to get to an ER to get imaged otherwise I could loose my left testicle. Turns out I had a double hernia. Since I was advised to go to ER by Tell-a-Doc the insurance company had to pay the ER bill. Company policy is ER is only covered in life and death situations.
Mike, I am very sorry to hear about your challenges. It is very frustrating when insurance companies deny medical care. I hope you are able to get this resolved.
I had an MRI a year ago which showed two lumbar herniated discs. At that point the discomfort was not that bad. Within the past two months I have had tremendous amount of pain in my back. My orthopedic doctor wanted me to get another MRI to determine if the herniations have gotten worse. Insurance denied the first request as well as the appeal by my doctor. I am paying for the MRI out of pocket because I don’t have a choice.
Lorraine, I am sorry to hear this. I hope you get relief from your pain.
My doctor said I needed an MRA on my kidney a week after I had been hospitalized for severe hypertension. I called and got it pre-authorized. I received a letter saying it was approved from my insurance company. I scheduled the MRA. Went to the appointment. Then 2 months later I got the EOB stating the claim was denied and a bill from the health care provider for $3,400!! My policy has $1,000 deductible (which I had prior to scheduling the MRA). I’m obviously going to fight this but would I start by going to my insurance company or to the health care provider that billed me for practically the entire cost of the MRA?
Hi Dan,
Based on what you have described I would start with your insurance company. The health care provider bills for the service. If it was pre-authorized by your insurance company, the error is likely on their end. The other possibility is that the bill was submitted by the provider with the wrong code. Either way, your insurance company should be able to provide an explanation. Good luck!
They have become so much expensive these days. Thank you for a detailed article on this topic, very useful information.
Thank you, Nicole Rochester, for sharing this article. The article is so much informative and detailed. The very first time when I was experiencing severe pain in my head, I didn’t know what I was going through. Hence, I consulted my doctor and he suggested undergoing a CT scan. After doing some research on radiology centers, I found a few online websites like labfinder.com, econolabs.com, etc. where I could select an option of my insurance provider and book an appointment instantly.
My insurance co approved my MRI do to cancer then when I did the MRI I received a letter of denial. What can I do
Hi John,
Hopefully, you received written (and not just verbal) notice of your insurance company’s approval. If so, I would email or fax that to the company as proof that you proceeded with the study based on information that the test was approved. Perhaps this was a clerical error on their part. Good luck!
Yikes, I thought my situation was bad, playing phone tag for a week to get a CT authorized at a place that’s in-network. But these other stories are much worse. I have a family history of cancer and I’m scared of this abdominal pain. I hope the delays aren’t allowing whatever it is to become worse.
Is anyone attempting to reform this system?
My mother fell and hit her head on a cement sidewalk. Since it was after 7 PM we took her to the ER. After a few hours they said they wanted to do a CT scan of her neck and head to make sure there were no problems there. After the scan they said she appeared to be okay and sent her home. Over a month later we get a bill for $739. They said the claim was denied because “These are non-covered serviced because this is a routine exam or screening procedure done in conjunction with a routine exam”. What is routine about falling and hitting your head on concrete???? It was not as if it were a part of a yearly physical. We spoke to Medicare and they said that they thought it could be a “coding” error. Mom has both Part A and B, and Blue Cross supplement that covers everything but a small deductible.
John, that is absolutely ridiculous! I’m so sorry. I hope you all have filed an appeal.
Yes, I went to the hospital and they were paid for the use of the facilities and the equipment. However, the radiologists bill separately, from what I now understand. The hospital agreed that it was crazy for a CT done as a result of a fall and a visit to the ER not to be covered by Medicare and mom’s Blue Cross supplement. They felt that it was likely a coding error. I called the office that handles the radiologists’ billing and they said yes, it looked like a coding issue. They are going to update it and resubmit. Hopefully that will end the matter. I have similar coverage for myself, and it makes me nervous to think I am well-covered but that I could get a nasty surprise if I had to make an emergency visit to the hospital.
You suggest to trust the doctor to decide whether a scan should be done at a hospital or free standing clinic. First. Are you saying that they would have different results.
Second. Most physicians send their own patients to the labs and, facilities that are contracted by their physician groups. Regardless of your insurance…which is a reminder to always preauthorize or check your own insurance coverage. Always.
Hi Deb,
The interpretation of the study may vary, depending on the experience of the radiologist. If the purpose of the scan is to compare the results to prior studies, having the study done at the same facility can be incredibly helpful. As an alternative, you could get a copy of the prior scans and give them to the radiologist at a free-standing facility. Also, there are laws in place that prevent physicians from referring patients to labs and facilities with which they have a financial relationship. (Although I’m not saying this does not happen.) Ideally, your physician should send you to facilities that are in-network for your health insurance plan.
Hi,
My doctor said I need 2 MRI’s for neck and chest. And I scheduled for the same. In between I got Precertification for both as well. Last minute change happened and instead of Chest MRI , hospital took CAT scan without Contrast (after doctors approval). But they missed to get Precertification. After lots of talk they started retro Authorization, but my insurance denied the case because hospital didn’t take pre-cerification prior to procedure. Now I am diagnosed with cancer, and have scheduled surgery. Instead of worrying all of these I am struggling with insurance, hospital and all.
Is there any solution to avoid all these?
Sgani, first let me say I am so sorry you have been diagnosed with cancer. Situations like this drive me nuts because you did everything you could possibly do. You made sure to get precertification for both tests, yet a last-minute change was requested (presumably based on something they saw on your initial scans). I would consider filing an appeal with your insurance company. You can read your plan benefits or contact a customer service rep for details about the process to follow. Also, read the section of your benefits manual that discusses pre-certifications and see if there are any exceptions are special circumstances that may apply to your situation. I wish you all of the best!
My husband had a referral for an x-ray and MRI…I called the hospital to make arrangements.. they checked all his insurance info… he didn’t need prior authorization… good to go… he had his test…5 days later we get a letter from insurance saying his procedure was not approved…i don’t understand
Lori, I’m so sorry to read this. The first step is to read the letter thoroughly to figure out why the procedure was not approved. Be sure to contact the insurance company if you have questions. I invite you to read my article “How to File an Appeal When Your Insurance Company Refuses to Pay (https://yourgpsdoc.com/2017/06/11/how-to-file-appeal-insurance/) for more information. In the future, always check with your insurance company prior to getting advanced radiology studies like CT and MRI scans. The hospitals are not always reliable. I hope you’re able to work this out.
Our PCP requested a CT Scan at the request of a radiologist who saw some concerning areas on my husband. He advised a CT Scan in 6 months. The PCP ordered the test and Cigna denied it on 03/16/2022. A blockage would have been visible on the CT Scan. Our PCP was contesting the denial when he suffered a sudden cardiac arrest on 04/20/2022 and died on 04/28/2022. If a preliminary test has already been performed and recommendations are given by a radiologist to follow up in 6 months with a CT Scan for multiple areas of concern why would the test be denied?
I have received a Denial from my insurance company for an MRI of my left knee. Been through the peer to peer and still denied. My question is if I pay for this myself to have it done, am I going to be paying my BCBS contract rate with the company? (Told it was 236.19) or would I be paying the Cash price the Outpatient Imaging company has? (Quoted at $450) Of course I would rather pay the 236.19, but does the mri company have to give me that price?
If the service is denied by your insurance company then you will not get the BCBS negotiated contract rate. I’m sorry it was denied.